|
|
|
|
|
Paediatric AFRS: Endoscopic Sinus Surgery: A Game Changer in Restoring Facial Cosmesis
|
|
|
|
Ramkumar Rethinasamy, Lokesh Kumar Penubarthi, Sabharisan Paramasivam Department of ENT, JIPMER, Pondicherry, India. |
|
|
|
|
|
Corresponding Author:
|
|
Dr. Lokesh Kumar Penubarthi Email: ramrethin10@gmai.com |
|
|
|
|
|
|
|
|
Received:
21-MAY-2023 |
Accepted:
30-OCT-2023 |
Published Online:
25-DEC-2023 |
|
|
|
|
|
|
|
Abstract
|
|
|
|
Background: Paediatric allergic fungal rhinosinusitis is a subtype of chronic rhinosinusitis with significant focus in the paediatric population owing to early onset and difficulty managing through adult treatment options. Case Report: A 13-year-old male presented with nasal obstruction and facial deformity persisting for ten months. Examination revealed polypoidal tissue in both nasal cavities. Imaging showed involvement of all paranasal sinuses with tissue changes extending to the pons and compressing the frontal lobe. Endoscopic sinus surgery, coupled with steroids, cleared the disease. Histopathology and fungal cultures indicated allergic fungal rhinosinusitis. Post-surgery, nasal symptoms resolved, and after six months, facial deformity improved without need for further cosmetic interventions, leaving the parents satisfied. Conclusion: This case report highlights the need for early surgical intervention and monitored use of peri-operative steroids in paediatric AFRS. |
|
|
|
|
|
Keywords :
|
Allergic Fungal Rhinosinusitis, Deformities, Nasal Cavity, Nasal Obstruction, Steroids.
|
|
|
|
|
|
|
|
|
|
|
|
Introduction
Allergic fungal sinusitis is a hyperintense response to fungi in the paranasal sinuses [ 1]. Paediatric allergic fungal sinusitis, even in extensive cases, can present with few symptoms. Other associated systemic diseases such as ciliary dyskinesias and cystic fibrosis must be ruled out in these cases. Special care is needed for children to treat the disease early, limit disfiguring sequelae, and avoid intracranial and intra-orbital complications. Timely treatment, with an emphasis on follow-up, is critical in cases of allergic fungal sinusitis.
Case Report
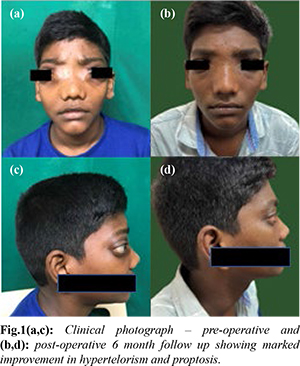
A 13-year-old male adolescent with no known medical co-morbidities presented with a chronic, progressive bilateral nasal obstruction for ten months, along with gross facial deformity and abaxial proptosis for six months. His visual acuity was within normal limits at six feet. Abaxial proptosis, which is the protrusion of the eyeball from the orbit, with increased interpupillary distance (hypertelorism) was noted on examination [Fig.1a,c]. On external examination of the nose, the nasal bridge was flattened and widened, a characteristic finding in patients with chronic rhinosinusitis with nasal polyps. The child had a hypo-nasal voice and was mouth-breathing most of the time due to the extensive blockage in his nasal cavities. Anterior rhinoscopy revealed that pale polypoidal tissue, which appeared as a mass of grape-like clusters, completely filled both nasal cavities. It did not bleed on touch and was insensitive, consistent with the diagnosis of nasal polyps. His visual acuity was 6/12 in both eyes, and extraocular movements were complete and symmetrical. Blood evaluation showed peripheral eosinophilia, with an absolute eosinophil count of 3570 cells/µL, indicative of an allergic reaction.
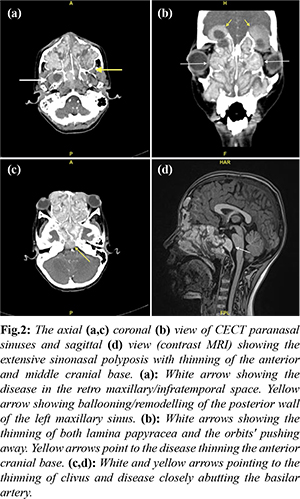
The patient's condition was evaluated using both contrast-enhanced computerized tomography (CECT) and contrast-enhanced magnetic resonance imaging (MRI). The imaging revealed a soft tissue density, which appeared as T1 hyperintense and T2 hypointense peripherally enhancing contents. The soft tissue density was observed to be expanding all sinus walls, causing thinning, remodelling, and occasional destruction with hyperattenuating areas noted within it [Fig.2a,b]. No apparent orbital involvement was seen, but a bulging lamina papyracea was present, indicating compression of the orbital tissues. The soft tissue density was posteriorly extending into the nasopharynx, pterygopalatine fossa, erosion of the posterior wall of the sphenoid sinus with extension into the brainstem into the pons region. It was also noted to be abutting the basilar artery, a major blood vessel supplying blood to the brainstem [Fig.2c]. The anterior cranial base was observed to be thinning as well [Fig.2b].
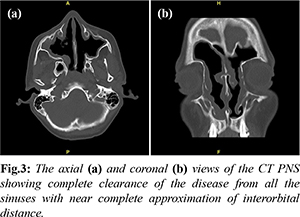
Prior to surgery, the patient was started on a tapering course of oral prednisolone for two weeks to manage the symptoms. During the surgery, we performed endoscopic clearance of the disease and widened all sinus ostia to provide proper ventilation and drainage. Vast deposits of eosinophilic mucin were found in all sinuses during the procedure. The post-operative biopsy revealed dense chronic inflammation comprising lymphocytes, plasma cells, and eosinophils with foreign body-type giant cells. The PAS (Periodic acid-Schiff) and GMS (Grocott-Gomori’s methenamine silver) stains highlighted short septate branching fungal hyphae consistent with Aspergillus species. However, there was no evidence of tissue or perivascular invasion. Fungal culture grew Aspergillus flavus. After the surgery, the patient showed remarkable improvement in nasal obstruction and epiphora. He was prescribed low-dose oral steroids for two weeks, topical steroid nasal spray, and nasal douching. The patient also underwent regular monthly follow-ups for endoscopic cleaning of sinuses. The six-month follow-up showed complete resolution of symptoms with the remodelling of facial bones [Fig.1b,d]. Additionally, the follow-up scan revealed total clearance of the disease from all sinuses [Fig.3].
Discussion
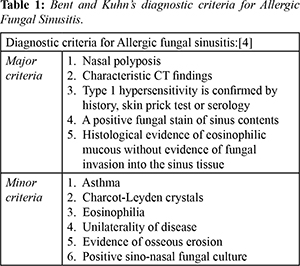
Allergic fungal rhinosinusitis (AFRS) is a non-invasive fungal sinusitis that is characterized by alterations in the innate immunity, type 2 inflammation with alteration in sino nasal adaptive immune response, and direct involvement of fungal elements in the pathogenesis [ 2]. Although AFRS is more commonly seen among adults, it can also occur in children, but there is a scarcity of literature on its clinical course in this age group [ 3]. Studies suggest that the clinical presentation of AFRS in children is subtle, with a slow onset of symptoms, and often involves facial dysmorphism [ 4, 5]. Facial deformities, proptosis, intra-orbital and intracranial extension, and an increased risk of recurrence are more commonly seen in children than in adults [ 6]. The pliable nature of the pediatric skeleton and the expansile force of allergic fungal sinusitis are believed to contribute to the higher incidence of facial deformities in children. AFRS is predominantly caused by dematiaceous fungi, including Bipolaris, Curvularia, Alternaria, and Drechslera species, with Aspergillus fumigatus being the most commonly reported Aspergillus species [7]. In this case, the fungal culture grew Aspergillus flavus. The diagnosis of AFRS can be made using Bent and Kuhn's criteria, which helps distinguish it from other forms of eosinophilic mucin chronic rhinosinusitis [Table 1] [2,4,8]. The child's clinical features met the criteria, which guided the diagnosis of AFRS and helped plan the appropriate treatment.
The management of AFRS is a multifaceted approach that involves both surgical and medical interventions. Pre-operative medical therapy is crucial in reducing inflammation and minimizing the burden of fungal antigens. Surgery is almost always necessary for patients with AFRS. Endoscopic sinus surgery has significantly reduced the chances of complications and recurrence. The primary objective of medical management is to attain long-term symptom control, limit the growth of polyps, and prevent the need for revision surgery. Various medical modalities are available, including systemic and topical steroids, leukotriene inhibitors, anti-fungal therapy, immunotherapy, and biological agents [9,10]. Although the efficacy of steroids in achieving the primary goals of medical treatment in AFRS is well-established, the role of anti-fungal and immunotherapy in AFRS is not well-defined in the literature. In the case presented, the patient underwent endoscopic surgery and systemic and topical steroid therapy. Due to the high risk of recurrence among children, regular follow-up sinus care and medical therapy are essential to prevent relapse.
Conclusion
Allergic fungal rhinosinusitis (AFRS) is a rare condition in children, which can lead to significant facial deformities, proptosis, intra-orbital and intracranial extension, and increased chances of recurrence. AFRS is managed with a combination of medical and surgical treatment, with pre-operative knowledge of the disease extent helping in precise intra-operative management. Tapering courses of peri-operative steroids play a pivotal role in pediatric AFRS. With appropriate management and follow-up, the chances of recurrence can be reduced, and the child can have a complete resolution of symptoms and remodelling of facial bones. Furthermore, educating parents and caregivers on the importance of regular follow-up visits and adherence to medical therapy can help prevent recurrences and improve outcomes for pediatric patients with AFRS.
Contributors: RR: manuscript writing, patient management; LKP: manuscript editing, patient management; SP: critical inputs into the manuscript. RR will act as a study guarantor. All authors approved the final version of this manuscript and are responsible for all aspects of this study. Funding: None; Competing interests: None stated.
References - Patro SK, Verma RK, Panda NK, Chakrabarti A. Understanding paediatric allergic fungal sinusitis: Is it more aggressive? Int J Pediatr Otorhinolaryngol. 2015;79(11):1876-1880.
- Tyler MA, Luong AU. Current concepts in the management of allergic fungal rhinosinusitis. Immunol Allergy Clin North Am. 2020;40(2):345-359.
- Alenzi HL, Al Momen A, Molani F. Pediatric allergic fungal rhinosinusitis with extensive intracranial extension – Case report and literature review. Int J Surg Case Rep. 2020;75:437-440.
- Thorp BD, McKinney KA, Rose AS, Ebert CS Jr. Allergic fungal sinusitis in children. Otolaryngol Clin North Am. 2012;45(3):631-642,
- McClay JE, Marple B, Kapadia L, Biavati MJ, Nussenbaum B, Newcomer M, et al. Clinical presentation of allergic fungal sinusitis in children. Laryngoscope. 2002;112(3):565-569.
- Gupta AK, Bansal S, Gupta A, Mathur N. Is fungal infestation of paranasal sinuses more aggressive in pediatric population? Int J Pediatr Otorhinolaryngol. 2006;70(4):603-608.
- Chhabra A, Handa KK, Chakrabarti A, Mann SB, Panda N. Allergic fungal sinusitis: clinicopathological characteristics. Mycoses. 1996;39(11-12):437-441.
- Ryan MW. Allergic fungal rhinosinusitis. Otolaryngol Clin North Am. 2011;44(3):697-710.
- Luk LJ, DelGaudio JM. Topical drug therapies for chronic rhinosinusitis. Otolaryngol Clin North Am. 2017;50(3):533-543.
- Marple BF. Allergic fungal rhinosinusitis: Surgical management. Otolaryngol Clin North Am. 2000;33(2):409-418.
|
|
|
|
|
|
|
Search Google Scholar for
|
|
|
Article Statistics |
|
Rethinasamy R, Penubarthi LK, Paramasivam SPaediatric AFRS: Endoscopic Sinus Surgery: A Game Changer in Restoring Facial Cosmesis.JCR 2023;13:125-128 |
|
Rethinasamy R, Penubarthi LK, Paramasivam SPaediatric AFRS: Endoscopic Sinus Surgery: A Game Changer in Restoring Facial Cosmesis.JCR [serial online] 2023[cited 2026 May 9];13:125-128. Available from: http://www.casereports.in/articles/13/4/Paediatric-AFRS.html |

|
|
|
|
|