6go6ckt5b8|3000F7576AC3|Tab_Articles|Fulltext|0xf1ff3437020000001e01000001001000
6go6ckt5b5idvals|172
6go6ckt5b5idcol1|ID
6go6ckt5b5|2000F757Tab_Articles|Fulltext
Oral submucosal fibrosis is a chronic, complex, irreversible, highly potent pre-cancerous condition characterized by juxta-epithelial inflammatory reaction and progressive fibrosis of the submucosal tissues. As the disease progresses, the jaws become rigid to the point that the sufferer is unable to open his mouth [1,2]. The condition is linked to oral cancer and is associated with areca nut chewing and tobacco chewing, which is practiced predominately in Southeast Asia and India. Intubation in patients with extensive submucosal fibrosis is an anaesthetic challenge, more so without the aid of fibreoptic bronchoscope.
A 55 year old male with deformed lower lip and restricted mouth opening came for preanaesthetic checkup. Patient had history of carcinoma lip which was operated twice, over a span of 3 years followed by cycles of radiotherapy for 2 months and was posted for lower lip reconstruction surgery. On examination of airway, mouth opening was ½ finger because of extensive submucosal fibrosis. Sternomental, thyromental and mentohyoid distance were normal. Lower incisors were missing [Fig.1]. All the routine investigations were within normal limit. We planned for awake nasal intubation and informed consent was taken from the patient. Preparation for emergency tracheostomy if required was done. Premedication was done with glycopyrollate and midazolam. Both nostrils were prepared with vasoconstrictive drops. Topical lignocaine 4% solution was applied to the nasal mucosa and sprayed in oral cavity. A 7.5 mm cuffed endotracheal tube (ETT) lubricated with lignocaine gel was introduced into the right nare with patients head in sniffing position. Air movements were continuously felt and heard while incrementally advancing the tube and cricoid pressure was applied to negotiate the tubes through the cords but such attempts failed as tube was sliding into oesophagus. The ETT was then connected to anesthetic circuit and ETCO2 monitor and withdrawn from oesophagus gradually, and stabilized at a position where ETCO2 curves and bag movements were visualized, we then passed a tube changer (with anteriorly curved tip) through the ETT which easily crossed the glottic opening [Fig.2]. Patient coughed which signaled us to slide the ETT over it. This time ETT passed successfully into the trachea. After removing tube changer, position of ETT was confirmed by capnography, chest auscultation and bag movements. Anaesthesia was induced with propofol, rocuronium and fentanyl and maintained with oxygen, nitrous oxide and desflurane. Intravenous hydrocortisone was given to reduce airway oedema due to repeated intubation attempts. After surgery residual neuromuscular blockade was reversed with neostigmine and glycopyrollate and patient was extubated. The whole perioperative course was uneventful.
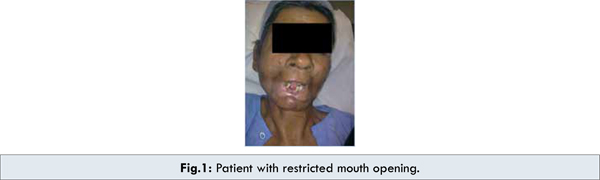
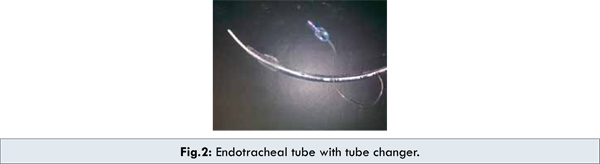
The American Society of Anesthesiologists (ASA) developed practice guidelines and an algorithm to assist anesthesiologists when faced with managing a difficult airway [3,4]. In conclusion, in the absence of fibreoptic bronchoscope where a difficult airway needs to be established, it depends on alternative clicks. In our case, a tube changer helped us in successful nasal intubation aided by capnography and bag movements. Regardless of which alternative is chosen an emergency, tracheostomy may be necessary for which all necessary preparation should be done in advanced.
References
- Cox SC, Walker DM . “Oral submucous fibrosis A review”. Aust Dent J London. 1996;41:294–299.
- Aziz SR . “Oral submucous fibrosis: an unusual disease”. J N J Dent Assoc. 1997;68:17–19.
- Practice guidelines for management of the difficult airway: a report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology. 1993;78:597.
- Practice guidelines for management of the difficult airway: an updated report by the American Society of Anesthesiologists Task Force on Management of the Difficult Airway. Anesthesiology. 2003;98:1269.