Introduction
Toxoplasmosis is the most common cause of posterior uveitis in the world and has the potential to cause blindness and visual impairment in children and young adults due to posterior segment abnormalities [
1-
3]. The typical manifestations show a retino-choroidal lesion located on macula while atypical manifestations are retrobulbar neuritis, pars planitis, papillitis, neuroretinitis, and retinal or choroidal neovascularizations [
2].
Neuroretinitis is a disease that is usually seen in young healthy adults in their first and second decades of life [
1,
2,
4]. Approximately 50% of the affected individuals experience an antecedent flu-like illness, usually affecting the upper respiratory tract [
4-
6]. Majority of cases are idiopathic, toxoplasmosis being a rare case [
3,
6,7]. The diagnosis from the ophthalmological findings can include optic nerve head edema, splinter hemorrhages, macular exudate in a stellate pattern, and various kinds of inflammation of the vitreous [
1,
2,
8]. Toxoplasmic antibody and serology testing is required in atypical manifestations to exclude idiopathic cases [
2]. The principal of treatment of ocular toxoplasmosis is to use drugs that can stop infection and inflammation [
9].
The purpose of this case series is to demonstrate two rare cases of unilateral neuroretinitis due to toxoplasmosis in children, which is a condition often overlooked by
ophthalmologists.
Case Report
Case 1
Our first patient was 10 year old boy who presented with chief complaint of sudden blurred vision of the left eye (LE) since last one month. There was no history of pain, redness, fever, eye disease, trauma, diabetes mellitus, hypertension, tuberculosis, asthma, tumor, or a scratch/bite by cats. One month before admission the patient was diagnosed with suspicious optic neuritis and was given oral methylprednisolone, 1x16 mg for 1 week with tapering the dose to 1x8 mg
from other hospital. The patient was referred to the neuro-ophthalmology division of RSCM Kirana due to non-improvement.
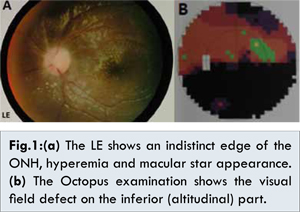
An ophthalmological examination of his LE revealed non-tender eye movements, with a visual acuity of 6/20 and normal intra-ocular pressure (IOP). Pupil was round, located centrally and test for rapid afferent pupillary defect (RAPD) was positive. There were cells in the vitreous and the funduscopy showed an indistinct edge of the pale optic nerve head (ONH), cup-to-disk ratio (CDR) could not be measured, artery-venous ratio 2/3, and a macular star appearance [Fig.1a]. The other parts were within normal limits. Octopus examination of the left eye showed a visual field defect on the inferior (altitudinal) part [Fig.1b]. Ophthalmological examination of right eye (RE)was unremarkable. The patient was diagnosed with neuroretinitis LE and was given methylprednisolone 1x8 mg. Follow up tests were planned to find risk factors.
One week after admission LE visual acuity was 6/9 with glasses; no other changes were detected. The toxoplasma IgG was positive, reaching 64 IU/mL (nonreactive value <1.0 IU/mL). The patient then consulted with the immunology division and was planned for fundus fluorescein angiography (FFA).Four weeks later the patient confirmed his vision was getting better; it was measured at 6/7.5. The FFA test showed early atrophy suspicious post-papillitis of LE. Methylprednisolone treatment was stopped, after which repeated tests of toxoplasma IgG and IgM were run, concluded with a consultation with the Pediatric Department to find other etiologies.
Six weeks after admissionthe IgG toxoplasmosis test showed a four fold rise in antibody titre (296.4 IU/mL). The visual acuity was 6/7.5, the anterior chamber was quiet and the RAPD was negative. The funduscopy showed an indistinct edge of the pale optic nerve head on the temporal site, cup-to-disk ratio could not be measured, the artery venous ratio was 2/3, and the macular star appearance had diminished [Fig.2]. The patient was diagnosed with neuroretinitis due to toxoplasmosis and asked to come in for a follow up appointment, but unfortunately he did not return before the creation of this report.
Case 2
A 12 year old female presented with chief complaints of sudden onset blurred vision and pain in LE since last 3 weeks. The pain did not increase on ocular movements and there was no history of red eye, nausea, vomiting, double vision or convulsions. One day before admission the patient had a fever and headache. There was no history of allergies, eye trauma, diabetes mellitus, hypertension, tumor, scratch or bite by cats or pulmonary tuberculosis or similar complaints in family members.
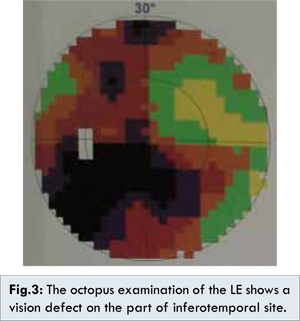
On ophthalmological examination of the LE visual acuity was 6/20. The pupil was round, located centrally and the RAPD was positive. The vitreous revealed cells and the funduscopy result showed the ONH had severe edema with an indistinct edge of >3/4 on the temporal part, hyperemia, cup-to-disk ratio could not be measured, arterio-venous ratio was 2/3, and the macular reflection was good. The Octopus examination of the left eye showed a visual field defect on the part of the infero-temporal site [Fig.3]. Other parts of the left eye, and the RE, were unremarkable. On general physical examination there were no lymphadenopathy or rashes, and the result of the remaining physical examination was also within normal limits.
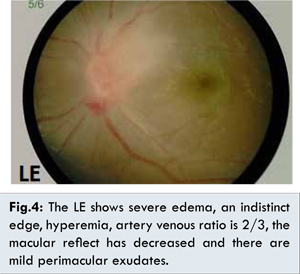
The patient was diagnosed with papillitis of the LE and referred to the neuro-ophthalmology (NO) division. In the NO division she was scheduled for an Octopus test for both eyes and hospitalized, to be treated with methylprednisolone 4x125 mg intravenously for three days. One day after therapy the visual acuity of the LE was 6/20. Fundus examination revealed that there was a splinter hemorrhage on the inferior optic nerve, a decrease of the macular reflect and exudates with macular star appearance [Fig.4]. Treatment was changed to oral methylprednisolone, and the patient was referred to the Infection and Immunology division and scheduled for TORCH tests.
The patient was diagnosed with neuroretinitis LE due to suspicious toxoplasmosis and given pyrimethamine 1x50 mg (1st day) and 1x25 mg (following days), cotrimoxazole 2x480 mg, methyl-prednisolone 1x16 mg, folic acid 1x1 tablet and weekly check-ups of leucocyte and thrombocyte levels. After several follow-up sessions within a period of 9 weeks, visual acuity and fundus appearance gradually improved from 6/18 to 6/7.5 with no RAPD. The funduscopy result showed an indistinct edge of ONH only on the temporal site [Fig.5-7]. The treatment was then stopped. Laboratory tests revealed reactive Toxoplasma IgG with an IgM of 2,709.0 IU/mL (reactive) and 0.5 IU/mL (non-reactive) respectively.
Two weeks after the treatment period the patient stated there were no more visual complaints. Visual acuity was 6/6 and the fundus examination showed an indistinct edge on the temporal side only.
Discussion
It is challenging to diagnose NR toxoplasmosis due to its rarity. The first challenge is to establish the diagnosis of NR, which can often be confused with the more common papillitis or papilledema. Funduscopy examination has several common features and can be interpreted wrongly by ophthalmologist [
5]. The second challenge is to decide the etiology of NR, as it is related to the management of the disease. Three literature studies [
3,
6,7] state that from all their patients with ocular toxoplasmosis (284 patients) only 0.70% (2 patients) was diagnosed with NR toxoplasmosis. In this case series, the diagnoses were established by clinical findings, serology tests and response to treatment.
The diagnosis of NR may be considered on initial examination based on acute unilateral visual loss with optic disc swelling, non-tender eye movements, a small degree of relative afferent pupillary defect, posterior vitreous cells (90% cases) and hard exudate arranged in a star figure around the fovea [
4,
10-
14]. Both patients discussed in this case series came to our clinic almost 3-4 weeks after the initial complaint. From the ophthalmological examination, visual acuitywas 6/20, the RAPD were positive, there were cells in the vitreous and the funduscopy results showed an indistinct edge of the pale optic nerve head (ONH), and a macular star appearance. This clinical finding appeared like NR even though Chipczyniska et al. [
11] stated that NR in children is a rare occurrence. The ophthalmology department initially diagnosed both patients with optic neuritis and papillitis.
The ancillary tests that help to confirm the diagnosis of NR are fluorescein angiography (FA) and visual field tests. The FA test from the first patient showed early atrophy which could be post-papillitis. This result caused some confusion about the diagnosis of the first patient. In NR, the FA will demonstrate a diffuse disc swelling and leakage of dye from vessels on the surface of the disc. The retinal vessels may show staining in the peripapillary region. But the most important point to note is the absence of leakage from the macular vasculature [
5,
15].
Visual field tests from both patients showed a visual field defect on the inferior site. The first patient showed an altitudinal field defect and the second patient showed an inferotemporal site field defect. Renuka et al. [
5] stated that visual field defects in NR might be cecocentral scotoma (the most common), central scotomas, arcuate defects, and even altitudinal defects may be present. These defects may be caused due to the occlusion of the posterior ciliary artery due to the edema of the optic nerve [
16].
The ocular toxoplasmosis diagnosis can be established by a funduscopy examination, but in atypical cases like ours, we need a complete work-up test to confirm the diagnosis [
17]. Another test that has diagnostic value for differentiation between recent and chronic infections is the IgG avidity test [
18]. Unfortunately, low IgG avidity values are not sufficient to identify an acute case of toxoplasmosis, but high avidity results can exclude a primary infection that was acquired up to five months earlier [
19]. However, detection of local antibody production from the aqueous or vitreous humour, examined with PCR, appears to be more useful in diagnosing ocular toxoplasmosis [
18]. Antibody detection from the aqueous or vitreous humour was not undertaken in the cases of this report. A common method to estimate the local versus systemic Toxoplasma-specific IgG is the Goldmann-Witmer coefficient [
20,
21]. Unfortunately these ancillary test are not available in our institution.
The serology test showed that the first patient had a negative result for IgM (0.3) but a positive result for Toxoplasma IgG (296.4). The second patient also showed a negative result for IgM, but Toxoplasma IgG showed a very reactive result (2709.0). Mantoux tests for both patients came out negative. These results show toxoplasmosis as the etiology of NR in both patients. This is based on literature that state that the etiology of NR due to toxoplasmosis can be made clear by the presence of serum IgM antibodies, or by the fourfold rise in IgG. Our results also show acute infection [
2,
22,
23] and is supported by the statement that IgG antibodies appear within the first 2 weeks after infection [
24].Ronday et al. [
25] suggested that an IgG titer of more than 300 IU is indicative of acute infection. In this case series, the elevation of antitoxoplasma antibodies (296.4 and 2709.0) was strongly suggestive of toxoplasmic NR [
13,
26].
There are several differential diagnoses for optic disk edema with macular star appearance, such as hypertensive retinopathy, papilledema, non-arteritic ischemic optic neuropathy (NAION), diabetic papillopathy, and disc and juxtapapillary tumors [
5,
10,
12,
15,
27]. From the general condition of both patients in this report there were not any vascular risk factors [
27]. The presence of vitreous cells also indicated NR rather than an infarct, as in 90% of NR cases posterior vitreous cells are usually present [
10]. Many infectious or non-infectious etiologies of NR can be the differential diagnosis, even though most cases of NR are idiopathic. The non-infectious causes include: systemic diseases, vascular diseases, diabetes, and cancer. The common infections that cause NR are cat-scratch disease, spirochetosis (especially syphilis), Lyme disease and leptospirosis. Cat-scratch disease accounts for two thirds of all cases [
12]. The etiology of NR can be discovered by means of anamnesis, clinical manifestation, serology tests or polymerase chain reaction (PCR) tests [
28]. From anamnesis the possible etiology is infectious. The infection etiology of the disease from both patients in this report is unlikely due to cat-scratch disease or Lyme disease, as there is no history of contact with cats, and the patients were not from an endemic area [
5]. The etiology of M. tuberculosis infection in NR should be considered, [
29] but there was no history of M. tuberculosis in our patients, which is supported by the negative Mantoux test results. A diagnosis of Leber’s stellate NR is given when there is no proven etiology of a disease, thus it is a diagnosis of exclusion made after other known causes of NR were ruled out [
5].
Efficacy of toxoplasmosis treatment in immunocompetent patients is debatable, but in this report’s cases of NR toxoplasmosis the prompt treatment with antibiotics and corticosteroids has shown to decrease inflammation and reduce subsequent damage to the optic nerve [
1,
8,
9,
30].Studies by Subshini et al. [
15], Hegab et al. [
22], and Paul et al. [
23] show that NR toxoplasmosis is a self-limiting disease in immunocompetent patients and lesions heal in 6-8 weeks without any treatment. However, Hegab et al. also state that permanent visual loss may eventually occur in these patients. This may be due to bilateral macular disease, papillomacular bundle or optic nerve involvement, retinal detachment, and possibly cataract. In our cases, different treatment was given to both patients. The second patient was given a combination of treatment, but the first patient was only treated with steroid. Our second patient was given pyrimethamine 1x50 mg the first day, continued with 1x25 mg the following days. Sulfadiazine was not given, but changed to cotrimoxazole 2x480 mg due to the availability in the hospital. Folic acid was also administered, and platelet and white blood cell counts were performed weekly, due to the side effects of the antimicrobial drugs [9,
23,
31].
To manage inflammation the second patient was given methyl-prednisolone 1x16 mg orally [21,30,32]. Even though the use of corticosteroid for treatment of ocular toxoplasmosis is considered controversial, we gave corticosteroids because the lesion threatened the optic disc. However, corticosteroids should not be used without concurrent antimicrobial agents, because it might lead to fulminant T. gondii infection [21,30,33]. The condition was different in our first patient: he was only given steroid therapy without anti-microbial drugs.
Paul et al. [
23] state that therapy is usually needed for 6 to 12 weeks in immunocompetent patients. Our second patient responded rapidly to anti-microbial and steroid treatment and showed significant improvement in visual acuity and fundus findings within 11 weeks after starting the therapy, even though there were still exudate appearances in the macula. This condition is similar to two literature cases, which state that exudates will disappear completely after a number of months (6-12 months), but often leaving residual subfoveal RPE defects in the macula. The disk edema from both patients had resolved, even though both disc appearances showed pallor and/or gliotic changes [4,5]. This visual field defect may still exist after treatment or resolution of the disease [
34].
Although we were unable to confirm our second patient’s diagnosis with histopathological evidence, the elevated four fold of antitoxoplasmosis antibody titers and the favorable responses to appropriate treatment were strongly suggestive of NR toxoplasmosis. Contrary to this case, our first patient had a reactive Toxoplasma serology result, but showed improvement without appropriate treatment the condition. From this condition we can conclude that the etiology from first patient may be idiopathic.
Conclusion
NR in children is a rare occurrence. Early diagnosis and treatment can prevent poor visual acuity. Even though the etiology of NR is usually idiopathic, Toxoplasma gondii infection should be considered in order to maintain visual acuity, by early diagnosis and a prompt therapy. To establish Toxoplasma infection serology tests should be evaluated, but in case the result is doubtful the diagnosis can be confirmed by the improvement of the condition with anti-Toxoplasma therapy.
References
- Cem K, Yonca A, Gurse Y. Ocular toxoplasmosis presenting as neuroretinitis: report of two cases. Ocular Immunology & Inflammation. 2002;10(3):229-234.
-
Atmaca L, Simsek T, Batioglu F. Clinical Features and Prognosis in Ocular Toxoplasmosis. Jpn J Ophthalmol. 2004;48:386-391.
-
Farzan K, Afsaneh NB, Zahra NB. Clinical manifestation and prognosis of active ocular toxoplasmosis in Iran. Int Ophthalmol. 2012;32:539-545.
-
Valerie P. Neuroretinitis. In: Albert DM, Miller JW, Azar DT, Blodi BA, Cohan JE, Tracy P, editors. Albert & Jakobiec’s Principles & Practice of Ophthalmology. 3rd ed. USA: Elsevier; 2008.1859-1863.
-
Renuka S, Subashini K. Neuroretinitis - Review. Kerala Journal of Ophthalmology. 2006;18:7-13.
-
Manuel GL, Lourdes AG. Ocular Toxoplasmosis: Clinical Characteristics in Pediatric Patients. Ocular Immunology & Inflammation. 2012;20(2):130-138.
-
Nicholas JB, Joao MF, Kevin LW, Justine RS. Ocular toxoplasmosis II: clinical features, pathology and management. Clinical and Experimental Ophthalmology. 2013;41:95-108.
-
Fish RH, Hoskins JC, Kline LB. Toxoplasmosis Neuroretinitis. Ophthalmology. 1993;100:1177-1182.
- David S, Uwe P. Uvea and Retina. In: David S, Uwe P, editors. Ocular Infection. 2nd ed. USA: Informa Healthcare; 2007:191-238.
-
Rana RG, Andrew GL. Optic Disk Edema With a Macular Star. Survey of Ophthalmology. 1998;43(3):270-274.
-
Chipczyniska B, Gra.ek M, Kepa B. Neuroretinitis in children: independent observations. Ann Acad Med Stetin. 2007;53:76-79.
-
Rakhshandeh A, Sima S. Acute papillitis in Young Female with Toxoplasmosis. Middle East African Journal of Ophthalmology. 2006;18(3):249-251.
-
Eckert GU, Melamed J, Menegaz B. Optic nerve changes in ocular toxoplasmosis. Eye. 2007;21:746-751.
-
Casson RJ, O’Day J, Fraco, Crompton JL. Leber fs idiopathic stellate neuroretinitis: Differential diagnosis and approach to management. Australian and New Zealand Journal of Ophthalmology. 1999;27:65-69.
-
Subashini K, Sunil N. Neuroretinitis: Update on a visual emergency and role of technology in its diagnosis. Journal Biomedical Science and Engineering. 2013;6:15-19.
-
Hayreh SS. Pathogenesis of visual field defects. British Journal Ophthalmology. 1970;54:289-311.
-
Ray S, Gragoudas E. Neuroretinitis. International ophthalmology Clinics. 2001;41(1):83-102.
-
Suresh S, Nor-Masniwati S, Nor-Idahriani MN, Wan-Hazabbah WH, Zeehaida M, Zunaina E. Serological IgG avidity test for ocular toxoplasmosis. Clin Ophthalmol. 2012;6:147-150.
-
Paul M. Immunoglobulin G Avidity in Diagnosis of Toxoplasmic Lymphadenopathy and Ocular Toxoplasmosis. Clinical And Diagnostic Laboratory Immunology. 1999;6(4):514-518.
-
Chapman DJ, Ashburn D, Ogston SA, Ho-Yen DO. The relationship between ocular toxoplasmosis and levels of specific toxoplasma antibodies. Epidemiol Infect. 1999;122:299-303.
-
Fatma A, Lembah R. Recent Advances in the Management of Ocular Toxoplasmosis. Southeast Asian J Trop Med Public Health. 2001;32:202-205.
-
Hegab SM, Al-Mutawa SA. Immunopathogenesis of toxoplasmosis. Clin Exp Med. 2003;3:84-105.
-
Paul Ng, Peter JM. Treatment of ocular toxoplasmosis. Aust Prescr. 2002;25:88-90.
-
Ophthalmology AAO. Intraocular Inflammation and uveitis. BSCS: Infectious Ocular Inflammatory Disease. San Fransisco, CA: American Academy of Ophthalmology, 2011: 226-235.
-
Ronday MJ, Ongkosuwito JV, Rothova A, Kijlstra A. Intraocular anti-toxoplasma gondii IgA antibody production in patients with ocular toxoplasmosis. Am J Ophthalmol. 1999;127:294-300.
-
Dina AJ, Jason RG, Laura JB. Inflammatory Optic Neuropathies and Neuroretinitis. In: Myron Y, Jay SD editors. Ophthalmology. 4th ed. USA: Elsevier Saunders; 2014:879-883.
-
Valerie P, Seema S, Aki K. Neuroretinitis: Review of the Literature and New Observations. Journal of Neuro-Ophthalmology. 2011;31:58-68.
-
Ferri FF. Ferri’s Clinical Advisor. 16th ed. Philadelphia: Mosby; 2014.
-
Stephen US, Robert YK, Emmet TC. Tuberculous Neuroretinitis. Journal of Neuro-Ophthalmology 1999;19(3):201-204.
-
Cristina M, Rubens B. Ocular Toxoplasmosis. In: Uwe P, Stephen F, editors. Uveitis and Immunological Disorders. 2nd ed. New York: Springer Berlin Heidelberg; 2007:131-134.
-
Daniel VV. Ocular toxoplasmosis. In: Myron Y, Jay SD, editors. Ophthalmology. 4th ed. USA: Elsevier Saunders; 2014:738-743.
-
Norman AS, Carly JS, Louis MW. Ocular Toxoplasmosis: Controversies in Primary and Secondary Prevention. J Neuroinfect Dis. 2013; 4:1-11.
-
Carlos EM, Daoling Z, Mandi DC, Gholam AP. Successful management of ocular toxoplasmosis during pregnancy using combined intraocular clindamycin and dexamethasone with systemic sulfadiazine. International Ophthalmology. 1999.