Sachin Gupta, Rohit Sharma, Nitin Saini, Yogeshwar Saini
Department of Orthopaedics, Sri Guru Ram Das Medical College, Amritsar 143001, India.
Corresponding Author:
Sachin Gupta
Email: dr.gupta.sachin@gmail.com
Abstract
Primary hyperparathyroidism revealed by a pathological fracture is very uncommon. We report a 47-year-old female patient with multiple pathological bone fractures. The diagnosis of primary hyperparathyroidism was made based on these bone changes and the elevated parathyroid hormone level. The histopathological findings confirmed the diagnosis of primary hyperparathyroidism with brown tumor. Patient was discharged in a stable condition with both fractures united six months after the surgery.
|
6go6ckt5b8|3000F7576AC3|Tab_Articles|Fulltext|0xf1ffc4a2010000006700000001001100 6go6ckt5b5idvals|141 6go6ckt5b5idcol1|ID 6go6ckt5b5|2000F757Tab_Articles|Fulltext Hyperparathyroidism is a disease of increased bone resorption and bone formation. Primary hyperparathyroidism is prevalent in approximately 1% of adult population and the usual causes are parathyroid adenoma, hyperplasia and, rarely, parathyroid carcinoma [1,2]. Brown tumor lesions caused by long-lasting primary hyperparathyroidism is a rare tumor-like lesion, often presenting with bone pain or by pathological fracture. We present the case of a 47 year old female who presented with multiple pathological fractures that led to the diagnosis of primary hyperparathyroidism.
Case Report
A 47-year-old lady presented to the outpatient department with history of fall in her house five days back. After fall patient had inability to bear weight on left lower limb and inability to use right arm. Radiographs confirmed a subtrochanteric fracture of left femur through an area of lytic bone and a mid shaft fracture of right humerus [Figure 1,2]. Plain radiographs of the hands, skull, and sacroiliac joints did not reveal any abnormality. The patient’s biochemical profile revealed markedly raised calcium of 3.7?mmol/l (normal range: 2.15–2.60) with normal creatinine levels. Her parathyroid hormone level was 970 ?pg/mL (normal range: 13–54) which was pointing towards the diagnosis of primary hyperparathyroidism. Ultrasound of the cervical region was done and it showed a hypoechoic adenoma deep in relation to lower pole of thyroid showing a parathyroid adenoma.
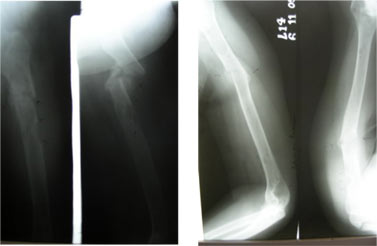
Figure 1: X ray AP and lateral view of subtrochanter fracture femur showing pathological fracture at subtrochanter level.
Figure 2: X ray AP and lateral view of shaft humerus showing pathological fracture at midshaft level.
The patient underwent proximal femoral nailing of left femur, plating of right humerus along with parathyroidectomy A large parathyroid weighing 15 gram was removed simultaneously [Figure 3]. The histological findings confirmed the diagnosis of an adenoma of the parathyroid [Figure 4]. Parathyroid tissue on histopathological examination was confirmed to be a benign parathyroid adenoma. There was a brief period of hypocalcemia which improved subsequently. Three weeks later, this was followed by a dramatic fall in serum PTH levels (52 ng/mL) and normalisation of serum calcium levels. Both the fractures united after six months.
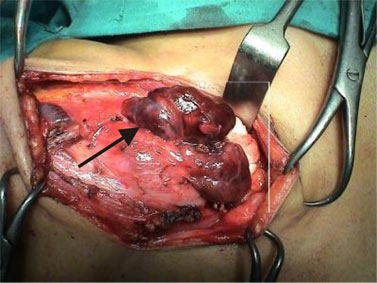 Figure 3: Shows macroscopic picture with arrow pointing over Parathyroid adenoma.
Figure 3: Shows macroscopic picture with arrow pointing over Parathyroid adenoma.
 Figure 4: Histopathological picture of parathyroid adenoma.
Discussion
Primary hyperparathyroidism may be asymptomatic or may present with severe metabolic disease –pathological fractures and renal calculi. Skeletal manifestations in the form of brown tumors are rare and according to literature occur in less than 2% of patients suffering from any form of hyperparathyroidism [1].
However, primary hyperparathyroidism presenting as a pathological fracture with no other systemic symptoms as in our case, is very uncommon [2]. Brown tumors are benign focal bone lesions caused by increased osteoclastic activity and fibroblastic proliferation, encountered in primary or more rarely secondary hyperparathyroidism [3]. These tumors are commonly found in the pelvis, ribs, sternum, femur, jaws and rarely the vertebrae [4]. Biochemical findings and clinical findings are very helpful in making the correct diagnosis. In our case the diagnosis of parathyroid adenoma was confirmed by histopathology. Brown tumours present radiographically as lytic lesions with regular borders. The cortices may be narrowed but there is no breach of cortex. Our patient’s radiologic views were also consistent with these findings. In addition to the surgical stabilization of the long bone fractures, aggressive treatment of hyperparathyroidism by removal of parathyroid adenoma is also necessary. The increased risk of fracture disappears following parathyroidectomy [5].
Conclusion
Brown tumor is a rare cause of pathological fractures. Stabilization of the fracture and removal of parathyroid adenoma are essential for treatment. This case report adds to the existing literature as it describes an unusual presentation of primary hyperparathyroidism.
References
Figure 4: Histopathological picture of parathyroid adenoma.
Discussion
Primary hyperparathyroidism may be asymptomatic or may present with severe metabolic disease –pathological fractures and renal calculi. Skeletal manifestations in the form of brown tumors are rare and according to literature occur in less than 2% of patients suffering from any form of hyperparathyroidism [1].
However, primary hyperparathyroidism presenting as a pathological fracture with no other systemic symptoms as in our case, is very uncommon [2]. Brown tumors are benign focal bone lesions caused by increased osteoclastic activity and fibroblastic proliferation, encountered in primary or more rarely secondary hyperparathyroidism [3]. These tumors are commonly found in the pelvis, ribs, sternum, femur, jaws and rarely the vertebrae [4]. Biochemical findings and clinical findings are very helpful in making the correct diagnosis. In our case the diagnosis of parathyroid adenoma was confirmed by histopathology. Brown tumours present radiographically as lytic lesions with regular borders. The cortices may be narrowed but there is no breach of cortex. Our patient’s radiologic views were also consistent with these findings. In addition to the surgical stabilization of the long bone fractures, aggressive treatment of hyperparathyroidism by removal of parathyroid adenoma is also necessary. The increased risk of fracture disappears following parathyroidectomy [5].
Conclusion
Brown tumor is a rare cause of pathological fractures. Stabilization of the fracture and removal of parathyroid adenoma are essential for treatment. This case report adds to the existing literature as it describes an unusual presentation of primary hyperparathyroidism.
References
- WeatherhallDJ, LedinghamJGG, WarrellDA, editors ; Oxford textbook of Medicine.
- 3rd ed Oxford University Press 1996; pp. 1630-1633
- Perez JA, Lopez B, Valdivia P, Norambuena L. Pathological fracture of femur due to Primary Hyperparathyroidism. Rev Med Chil 1989;117:1018-1022
- G.Bullough. “Neoplastic Diseases Of Bone” in Sternberg’s Diseases of Surgical Pathology; S.E. Mills, Ed Vol. 1, pp 245-264.
- Kanaan I, Ahmed M, Rifai A, Alwatban J. Sphenoid Sinus brown tmour of secondary Hyperparathyroidism: case report. Neurosurgery 1998; 42: 1374-1377.
- G Suchecki, B. Szudejko, “ Diagnostic Difficulties in Primary Hyperparathyroidisma case report,” Chirurgia Narzadow Ruchu I Orthopedia Polska 1999;l64:81-83.
|