6go6ckt5b8|3000F7576AC3|Tab_Articles|Fulltext|0xf1ffe44d310000008406000001000500
6go6ckt5b5idvals|2039
6go6ckt5b5|2000F757Tab_Articles|Fulltext
Introduction
Emphasis on anatomic reduction of forearm fractures and strict adherence to stable fixation techniques have reduced the rate of non-unions in the forearm to less than 3% [
1]. Open injuries, highly comminuted fractures, significant soft-tissue injury, inadequate surgical fixation, and infection are known predisposing factors to forearm non-unions [
1,
2]. The infected non-unions in the forearm are rare and the problem is complex due to the presence of bone necrosis, segmental bone loss, sinus tract formation, fracture instability, and scar adhesion of the soft tissues [
2,
3]. A large diaphyseal, segmental bone defect is a challenging problem in orthopaedic practice. Very few reports in the literature are available deliberating on the treatment strategies and functional outcomes [
1,
2]. Procedures used in the reconstruction of segmental defects of both bones of the forearm should, whenever possible, preserve forearm pronation and supination.
Case Report
A nineteen-year-old male patient presented to our department with post-traumatic infected gap non-union of middle two third and lower one third region left radius with a discharging sinus. He was previously operated elsewhere and was found to have undergone repeated surgical interventions.
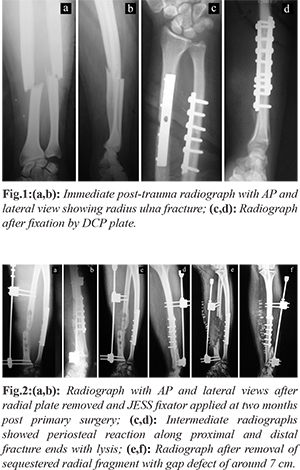
There was history of fall at home four months back sustaining a middle third and lower third junction forearm fracture of radius and ulna at the same level [Fig.1a,b]. Surgical stabilization by narrow 3.5 DCP plate was done for both fractures at a health care facility elsewhere on second day of injury [Fig.1c,d]. Infection and discharge from radial end ensued within three weeks of primary surgery. Antibiotic and regular dressings were unable to control discharge. Persistence of discharge followed for two months. Secondary procedure of radial plate removal, debridement and JESS distractor application was done [Fig.2a,b]. Radiograph revealed sequestration of radial segment under the plate with lysis along screw holes with periosteal reaction [Fig.2c,d]. Redo debridement under antibiotic coverage along with removal of sequestrum from radius followed creating a radial gap defect of around 7 cm [Fig.2e,f]. It was followed by six weeks of appropriate antibiotic therapy.
Patient presented to us after four months of his index surgery with persistence of low-grade infection with a discharging sinus and compounded by tissue cicatrisation, joint contractures of thumb and wrist with muscle wasting. The sinus was situated in the centre of the previous surgical wound. Radiograph revealed loss of radial segment of approximately 7 cm length, JESS distractor in radius and ulnar plate in situ with loss of radial dominance at wrist. At the time of presentation, he was found to have sterile culture reports, normal leucocyte count with elevated levels of ESR and CRP. Range of elbow movements was full. Forearm movements were painful allowing only 20° pronation. Evidence of low-grade pin tract infection was present.
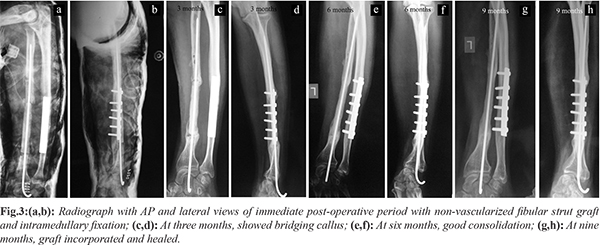
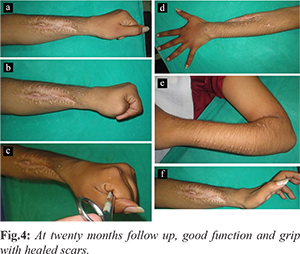
After initial management with debridement and antibiotics for 3 weeks, repeat ESR and CRP were normal. Indigenous method consisting of ipsilateral free non-vascularized fibular graft with a Kirshner wire fixation through the graft to restore the length of radius was done [Fig.3a,b]. Under general anaesthesia, the forearm external fixator was removed first. The surgical wound track which previously got infected was then cleared with thorough debridement until the graft bed appeared red and bled freely, along with appropriate antibiotic. The proximal and distal stump ends were cut to create raw fresh vascularized bony ends. Both ends were drilled retrograde with 2.7 mm drill bit to open medullary cavity. The bone gap was measured intra-operatively to 10 cm. Now the ipsilateral fibular graft of approximately 12 cm was harvested. The block of graft taken was trimmed at both ends to have long block of graft of desired length. The block was then reamed eccentrically with a 2 mm Kirshner wire through and through its longitudinal axis. A smooth K-wire of determined length was passed into the distal fragment of radius and as the wire protruded out through the distal stump the fibular graft was threaded on to the wire. As soon as it protruded out through the other end of the graft, the proximal fragment reduced over the wire with angulation and distraction techniques. Ipsilateral autologous cancellous bone chips were added to both fracture ends. Haemostasis was achieved and all wound were closed. Post-operatively above elbow slab was given for a period of two weeks with conversion to cast for another four weeks. The patient was encouraged active finger movements and was serially followed up with radiographs at three months interval [Fig.3c,d] showed bridging callus, at six months interval [Fig.3e,f] showed consolidation. At the end of nine months post operatively evidence of union was found at both ends of the graft [Fig.3g,h] with loss of radial dominance. At twenty months post-operative status patient regained satisfactory forearm and hand functions for his daily activities [Fig.4a-f]. There was no graft fracture. The patient was offered corrective procedure with ulna shortening, step cut osteotomy and re-plating, to restore the radial dominance. However, he did not consent for further intervention as his daily activities were painless and comfortable.
Discussion
Non-union can be caused by factors such as comminution or segmental fractures, bone defects, interposition at the fracture site, disruption of the blood supply in the fracture fragments, inadequate stabilization and local infection [
1,
4]. Problems involved in bridging or regenerating areas of skeletal loss with viable bone while maintaining limb length and alignment, along with satisfactory function remains a substantial challenge [
5]. The options for defect management include autogenous cancellous bone graft, autogenous cortico-cancellous bone graft and vascularized bone grafts (typically for the radius) in atrophic non-union [
1]. Surgical treatment aims to regain proper length, restore the anatomy and recover function of the forearm [
2,
4,
5,
6].
Non vascularized fibular graft is used to manage a diaphyseal forearm gap defect. It is a long, tubular, strong autogenous bone graft readily available [
7]. Sacrifice of the fibula does not appear to have any detectable functional disadvantage and donor site morbidity [
7-
9]. Clinical studies have suggested that the distal six cm of fibula should be preserved to maintain lateral stability of the ankle [
3,
5.
7]. The various studies found no correlation between the length of the non-vascularized fibular graft and the rate of healing.
Success of operative procedures involving non-vascularised autogenous bone graft depends on the ability of the surrounding soft tissues to withstand the operative manipulation and to re-vascularise the transplanted bone graft [
8]. Despite a high success rate, the danger of resorption, a high incidence of stress fractures, and the lack of biological activity have been thought to be disadvantages of non-vascularized fibular grafts compared to vascularized grafts [1,7,9]. Though vascularised grafts are significantly stronger than conventional fibular grafts however, graft fracture are known to occur in both [
5,
8]. In addition, donor site morbidity following graft or flap procedures should also be considered.
Illizarov bone transport procedures have provided alternatives for the reconstruction of composite skeletal and soft-tissue defects; however, such procedures are complex and lengthy and have been associated with many complications [
7,
8]. We achieved defect filling with osteo-inductive cortico-cancellous iliac crest graft and osteo-conductive fibular graft block and internal fixation by nail imparting stability to the fracture. In our procedure removal of nail does not require re-exposure of graft area. We used less metallic implant material which is advantageous over plating. The procedure allowed early rehabilitation. Nailing proved a useful option in our patient. We agree that strong and stable fixation is must for achieving union and locking plates are more preferred over conventional non-locking plates with bi-cortical locked screw purchase though their superiority remains questionable [
1,
7]. Adjacent soft tissue viability and potential for the coverage of implant by native tissues are considerations in choosing an implant. The patient was apprehensive after failure with a plate and it challenged the decision making for implant selection.
One of the important factors in achieving functional success is the restoration of radial bowing [
4]. Using a free non-vascularised fibular graft, excellent results in two cases of segmental ulnar defect with an average length of 9 cm were achieved [
8]. The Nicoll’s technique of cortical iliac graft with plating is recommended only in the absence of infection and if the bony gap does not exceed 50 mm [
4]. We modified Nicoll’s technique by using a flexible nail for fixing the graft. Also, we applied this method for a bone defect of 10 cm which is more than the proposed upper limit of fixation.
There are few reports to suggest superiority of any treatment options advocated. Successful outcome makes this a useful alternative in treatment of infective non-unions. We comprehend that significant challenges may arise with graft collapse, resorption and failure necessitating considerations of other treatment modalities.
Conclusion
Surgeons should opt for a treatment modality in an infected diaphyseal gap non-union of forearm considering challenges in securing a healthy surgical bed for reconstruction, selection of graft options for defect management and use of implant for secure fixation. The asepsis protocol should be adhered to in a primary surgery. We require simplifying the complex problem, and making it economically viable and easily reproducible.
Contributors: LT: conceptualization, patient management; GG: data collection, manuscript writing, patient management; PD: manuscript editing. GG will act as a study guarantor. All authors approved the final version of this manuscript.
Funding: None; Competing interests: None stated.
References
- Kloen P, Buijze GA, Ring D. Management of forearm nonunions: current concepts. Strat Traum Limb Recon. 2012;7:1-11.
- Prasarn ML, Ouellette EA, Miller DR. Infected nonunions of diaphyseal fractures of the forearm. Arch Orthop Trauma Surg. 2010;130:867-873.
- Nazim M, Nizamuddin MK. Fibula bone grafting in infected gap non-union: A prospective case series. National Journal of Clinical Orthopaedics. 2019;3(1):6-10.
- Venkateswarlu BSS, Manikumar CJ. Infected gap non-union of radius treated with modified Nicoll’s technique: A case report. Journal of Clinical and Diagnostic Research. 2015;9(2):RD01-RD02.
- Shah KB, Kamath J, Jayasheelan N, Danda R, Rai MK. Non-vascularized fibular strut grafting in management of bone defects. Online J Health Allied Scs. 2015;14(4):14.
- Parihar M, Ahuja D. Infected Nonunion of radius and ulna – Strategy of approach. Journal of Orthopaedic Case Reports. 2012;2(4):26-31.
- Nataraj B, Singh V, Pathak AC, Jain M, Khapane V. Non-vascularized fibula and corticocancellous bone grafting for gap nonunion of lower limb-retrospective study of 18 cases an age-old technique revisited. Eur Orthop Traumatol. 2014;5:277-283.
- El-Sayed M, El-Hadidi M, El-Adl W. Free non-vascularised fibular graft for treatment of post-traumatic bone defects. Acta Orthop. Belg. 2007;73:70-76.
- Mahdi M, Hafidh A. Free non-vascularized fibular graft in treatment of bone defects. Bas J Surg. 2007;13:69-75.