Rajesh Sinha, Abhijeet Kumar Jha, Smita Prasad
From the Department of Dermatology, STD & Leprosy; All India Institute of Medical Sciences, Patna; 801105, India.
Corresponding Author:
Dr. Rajesh Sinha
Email: sinhaderma@gmail.com
Abstract
Ciprofloxacin is a commonly used flouroquinolone antibiotic. We report a case of serum sickness like drug reaction due to ciprofloxacin. Serum sickness like reaction is a cutaneous adverse drug reaction to various drugs. It presents as fever, cutaneous rash and arthralgia. Common drugs implicated in causing serum sickness like drug reaction include penicillins, cephalosporins and tetracyclines. We report a case of serum sickness like reaction due to ciprofloxacin in a 13 year old boy, who was prescribed oral ciprofloxacin by a local practioner for furunculosis.
|
6go6ckt5b8|3000F7576AC3|Tab_Articles|Fulltext|0xf1ff3000060000005303000001001800 6go6ckt5b5idvals|394 6go6ckt5b5|2000F757Tab_Articles|Fulltext Introduction
Serum sickness was first described by Von Pirquet and Schick in 1905, describing fever, skin eruptions (mainly consisting of urticaria), joint pain, and lymphadenopathy in regions draining the site of injection after patients were given antitoxin in the form of horse serum [1]. The disease was common in the pre-antibiotic era when heterologous antiserum was used as passive immunization to treat infectious and toxic illness [2]. Now a day’s serum sickness like reaction though rare has been reported due to drugs that include most commonly penicillins and cefalosporins [3-4]. To the best of our knowledge, only 2 cases of ciprofloxacin induced serum sickness has been reported in literature [5-6]. Herein we report a case of ciprofloxacin induced serum sickness like reaction in a 13 year old boy.
Case Report
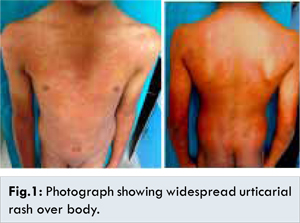
A 13 year old boy presented to the dermatology OPD with generalized erythematous rash, following intake of some medication for furunculosis by a local practioner. His further history revealed that he was taking oral ciprofloxacin for last six days. The patient also complained of fever, itching and joint pain. On examination, there was diffuse erythematous urticarial rash all over the body [Fig.1]. Urticarial polycyclic wheals were present on trunk, arms, legs and face. He also complained of mild burning and itching sensation. Skin examination did not reveal presence of any fungal or ectoparasite infestation. There was no history of such type of eruptions in the past. Diascopy showed blanching of the lesions. Dermatographism could not be demonstrated on patient’s skin. Family history did not reveal any history of allergic disease, urticaria or asthma in first degree relatives. Systemic examination did not reveal any abnormality except for fever (oral temperature of 102.6° F). Laboratory investigation showed raised ESR (36 mm/hr), normal white blood cell (WBC) count of 9600/µL with 64% neutrophils, 30% lymphocytes, 3% eosinophils, 2% basophils and 1% monocytes; hemoglobin 12.5 gm/dL, haemtocrit 36% and platelet count was 3,80,000/mm3. Blood urea nitrogen was 8 mg/dL and serum creatinine was 0.7 mg/dL. Total protein was 5.2 gm/dL, albumin 3.3 gm/dL, and blood culture was negative. Liver function test results were also within normal limits except for mild elevation of serum glutamic oxaloacetic transaminase level of 102 U/L and a serum glutamic pyruvic tranaminase level of 98 U/L. Serum IgE level was 36 IU/mL. The tests for antinuclear antibody, anti-dsDNA, hepatitis B surface antigen and antibody were negative. Routine urine examination was normal and culture showed no growth. A clinical diagnosis of drug induced serum sickness like reaction was made. The drug was stopped immediately. The patient was treated with hydroxyzine 10 mg daily and oral steroids 1 mg/kg/day. Within 24 hours of institution of therapy and stopping ciprofloxacin there was marked response in the patient’s condition.
Serum sickness was first described by Von Pirquet in 1905 following the use of antidiphtheria horse serum. The disease was common in the pre-antibiotic era when heterologous antiserum was often used as passive immunization to treat infectious and toxic illnesses [7]. Serum sickness is a type 3 hypersensitivity reaction. Symptoms occur coincidentally with the appearance of antibody formed against the injected antigen when latter is still present in the circulation. Immune complexes formed under conditions of moderate antigen excess lodge in small vessels and in filtering organs throughout the body. These complexes activate the complement sequence giving rise to the clinico-pathological manifestations [8]. Serum sickness is a clinical syndrome characterized by fever, lymphadenopathy, arthralgias, cutaneous eruptions, gastrointestinal disturbances, and malaise and is often associated with proteinuria. In contrast, serum sickness-like reaction (SSLR) is defined by the presence of fever, rash (usually urticarial) and arthralgias occurring 1-3 weeks after drug initiation. Other findings such as lymphadenopathy and eosinophlia may also be present. However immunecomplexes, hypocomplementemia, vasculitis, and renal lesions are absent in SSLR [9]. Common drugs implicated in causing serum sickness like reaction include penicillins, cephalosporins (particularly cefaclor), minocycline, bupropion and rituximab [9]. Ciprofloxacin, a fluroquinolone antibiotic can also rarely induce serum sickness like reaction. The earliest report of serum sickness-like reaction associated with ciprofloxacin was reported by Slama TG in 1990 [5]. He reported a case of 56 year old male who developed generalized urticarial eruption, severe polyarthralgia, and myalgia 4 days after taking ciprofloxacin. In our case, SSRL developed 5 days after taking ciprofloxacin. SSLR can occur 1 to 4 weeks after taking the inciting agent. Transient increase in liver enzymes levels can occur with ciprofloxacin. Mild elevation of liver enzymes was present in our case which subsided at 4 weeks follow up. Though arthralgia was present in our case there was no sign of joint effusion as described by Slama TG in his case report. Another case due to ciprofloxacin has been reported by Guhary SR [6]. He reported a case of 62 year old female who developed polyarthralgia, myalgia and a generalised urticarial rash following 5 days use of ciprofloxacin. Its differential diagnoses include drug hypersensitivity syndrome and erythema multiforme. Drug hypersensitivity syndrome manifests as morbiliform rash. In severe cases, erythroderma, purpura and extensive skin sloughing may occur. Anticonvulsants are commonly implicated in drug hypersensitivity syndrome. Erythema multiforme can be differentiated by presence of typical targetoid or iris lesion. The treatment of serum sickness like drug reaction mainly consists of discontinuation of the drug and antihistamines. A short course of oral corticosteroid may be required in patients with more severe symptoms. The drug causing SSLR should be avoided in future.
Conclusion
Ciprofloxacin is a commonly used oral antibiotic. Pubmed search showed only two cases of ciprofloxacin induced serum sickness like reaction has been reported. It may be a possibility that majority of these reactions are unrecognized and have not been reported. This case is being reported to emphasize the need for increased clinical awareness of such side effect, so that inciting agent can be discontinued and proper management be initiated as early as possible.
References
- Von Pirquet C, Schick B. Die Serumkrankheit Vienna, Franz Deuticke, 1905. (Translated into English by Schick in 1927.).
- Keeffe DT, Cooke R. Serum sickness like reaction in an 11-year-old boy. Ir J Med Sci. 2011;180(2):605-606.
- Katta R, Anusuri V. Serum sickness-like reaction to cefuroxime: a case report and review of the literature. J Drugs Dermatol. 2007;6(7):747-748.
- Vial T, Pont J, Pham E, Rabilloud M, Descotes J. Cefaclor-associated serum sickness- like disease: eight cases and review of the literature. Ann Pharmacotherapy. 1992;26(7-8):910-914.
- Slam TG. Serum sickness-like illness associated with ciprofloxacin. Antimicrob Agents Chemother. 1990;34:904-905.
- Guharoy SR. Serum sickness secondary to ciprofloxacin use. Vet Hum Toxicol. 1994; 36:540-541.
- Chao YK, Shyur SD, Wu CY, Wang CY. Childhood serum sickness: a case report. J Microbiol Immunol Infect. 2001;34(3):220-223.
- Roujeau JC, Stern RS. Severe adverse cutaneous reactions to drugs. N Engl J Med. 1994; 33:1275-1285.
- Knowles SR, Shear NH. Major adverse cutaneous effects from systemic drugs. In: Wolverton SE, 3rd ed. Comprehensive dermatologic drug therapy. Elsevier; 2013:749-750.
|